Abortion Side Effects | Abortion Dangers – After Abortion
Physical Side Effects Associated With Abortion
Printable Fact Sheets
Psychological Complications
More articles on abortion complications
Approximately 10% of women undergoing induced abortion suffer from immediate complications, of which one-fifth (2%) were considered major.19 However the majority of complications take time to develop and will not be apparent for days, months or even years.
Negative psychological reactions to abortion are more common than physical complications. These are described in a later section.
The major physical risks and complications of abortion are described below. Citations to the medical literature regarding each danger or risk are included as end notes at the bottom of this page.
ELEVATED RISK OF DEATH
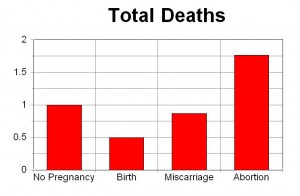
According to the best record based study of deaths following pregnancy and abortion, a 1997 government funded study in Finland, women who abort are approximately four times more likely to die in the following year than women who carry their pregnancies to term. In addition, women who carry to term are only half as likely to die as women who were not pregnant.16 (Click here for more details on this important study.)
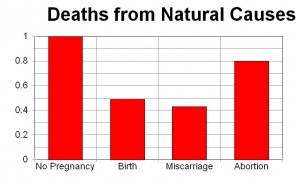
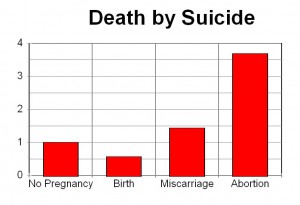
The Finland researchers found that compared to women who carried to term, women who aborted in the year prior to their deaths were 60 percent more likely to die of natural causes, seven times more likely to die of suicide, four times more likely to die of injuries related to accidents, and 14 times more likely to die from homicide.
Researchers believe the higher rate of deaths related to accidents and homicide may be linked to higher rates of suicidal or risk-taking behavior.16 (Click here for details on the latest research regarding abortion associated deaths.)
The leading causes of abortion related maternal deaths within a week of the surgery are hemorrhage, infection, embolism, anesthesia, and undiagnosed ectopic pregnancies. Legal abortion is reported as the fifth leading cause of maternal death in the United States, though in fact it is recognized that most abortion-related deaths are not officially reported as such.2 (Click here for more details on the underreporting of abortion related deaths in the U.S.)
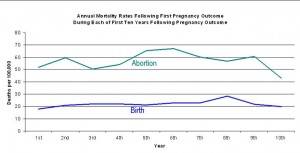
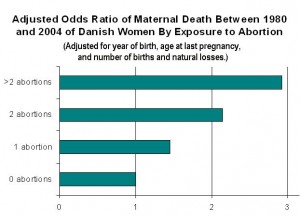
Two studies of the entire population of women in Denmark published in 2012 have shown similar results. The first found that the risk of death following abortion remains higher in each of the first ten years following the abortion. The second found that the risk of death increases with each abortion, 45% after one abortion, 114% after two abortions, and 192 percent after three or more abortions.
For a complete review of the literature see Deaths associated with abortion compared to childbirth: a review of new and old data and the medical and legal implications (2004).
CERVICAL, OVARIAN, AND LIVER CANCER
Women with a history of one abortion face a 2.3 times higher risk of having cervical cancer, compared to women with no history of abortion. Women with two or more abortions face a 4.92 relative risk. Similar elevated risks of subsequent ovarian and liver cancer have also been linked to single and multiple abortions. These increased cancer rates for post-aborted women may be linked to the unnatural disruption of the hormonal changes which accompany pregnancy and untreated cervical damage or to increased stress and the negative impact of stress on the immune system.4
UTERINE PERFORATION
Between 2 and 3% of all abortion patients may suffer perforation of their uterus, yet most of these injuries will remain undiagnosed and untreated unless laparoscopic visualization is performed.5 Such an examination may be useful when beginning an abortion malpractice suit. The risk of uterine perforation is increased for women who have previously given birth and for those who receive general anesthesia at the time of the abortion.(6) Uterine damage may result in complications in later pregnancies and may eventually evolve into problems which require a hysterectomy, which itself may result in a number of additional complications and injuries including osteoporosis.
CERVICAL LACERATIONS
Significant cervical lacerations requiring sutures occur in at least one percent of first trimester abortions. Lesser lacerations, or micro fractures, which would normally not be treated may also result in long term reproductive damage. Latent post-abortion cervical damage may result in subsequent cervical incompetence, premature delivery, and complications of labor. The risk of cervical damage is greater for teenagers, for second trimester abortions, and when practitioners fail to use laminaria for dilation of the cervix.7
PLACENTA PREVIA
Abortion increases the risk of placenta previa in later pregnancies (a life threatening condition for both the mother and her wanted pregnancy) by seven to fifteen fold. Abnormal development of the placenta due to uterine damage increases the risk of fetal malformation, perinatal death, and excessive bleeding during labor.8
SUBSEQUENT PRE-TERM DELIVERIES AND OTHER COMPLICATIONS OF LABOR
Women who had one, two, or more previous induced abortions are, respectively, 1.89, 2.66, or 2.03 times more likely to have a subsequent pre-term delivery, compared to women who carry to term. Prior induced abortion not only increased the risk of premature delivery, it also increased the risk of delayed delivery. Women who had one, two, or more induced abortions are, respectively, 1.89, 2.61, and 2.23 times more likely to have a post-term delivery (over 42 weeks).17 Pre-term delivery increases the risk of neonatal death and handicaps.
HANDICAPPED NEWBORNS IN LATER PREGNANCIES
Abortion is associated with cervical and uterine damage which may increase the risk of premature delivery, complications of labor and abnormal development of the placenta in later pregnancies. These reproductive complications are the leading causes of handicaps among newborns.9
ECTOPIC PREGNANCY
Abortion is significantly related to an increased risk of subsequent ectopic pregnancies. Ectopic pregnancies, in turn, are life threatening and may result in reduced fertility.10
PELVIC INFLAMMATORY DISEASE (PID)
PID is a potentially life threatening disease which can lead to an increased risk of ectopic pregnancy and reduced fertility. Of patients who have a chlamydia infection at the time of the abortion, 23% will develop PID within 4 weeks. Studies have found that 20 to 27% of patients seeking abortion have a chlamydia infection. Approximately 5% of patients who are not infected by chlamydia develop PID within 4 weeks after a first trimester abortion. It is therefore reasonable to expect that abortion providers should screen for and treat such infections prior to an abortion.11
ENDOMETRITIS
Endometritis is a post-abortion risk for all women, but especially for teenagers, who are 2.5 times more likely than women 20-29 to acquire endometritis following abortion.12
IMMEDIATE COMPLICATIONS
Approximately 10% of women undergoing elective abortion will suffer immediate complications, of which approximately one-fifth (2%) are considered life threatening. The nine most common major complications which can occur at the time of an abortion are: infection, excessive bleeding, embolism, ripping or perforation of the uterus, anesthesia complications, convulsions, hemorrhage, cervical injury, and endotoxic shock. The most common “minor” complications include: infection, bleeding, fever, second degree burns, chronic abdominal pain, vomiting, gastro-intestinal disturbances, and Rh sensitization.13
INCREASED COMPLICATIONS FOR WOMEN SEEKING MULTIPLE ABORTIONS:
In general, most of the studies cited above reflect risk factors for women who undergo a single abortion. These same studies show that women who have multiple abortions face a much greater risk of experiencing these complications. This point is especially noteworthy since approximately 45% of all abortions are for repeat aborters.
LOWER GENERAL HEALTH:
In a survey of 1428 women researchers found that pregnancy loss, and particularly losses due to induced abortion, was significantly associated with an overall lower health. Multiple abortions correlated to an even lower evaluation of “present health.” While miscarriage was detrimental to health, abortion was found to have a greater correlation to poor health. These findings support previous research which reported that during the year following an abortion women visited their family doctors 80% more for all reasons and 180% more for psychosocial reasons. The authors also found that “if a partner is present and not supportive, the miscarriage rate is more than double and the abortion rate is four times greater than if he is present and supportive. If the partner is absent the abortion rate is six times greater.” (15)
This finding is supported by a 1984 study that examined the amount of health care sought by women during a year before and a year after their induced abortions. The researchers found that on average, there was an 80 percent increase in the number of doctor visits and a 180 percent increase in doctor visits for psychosocial reasons after abortion.18
INCREASED RISK FOR CONTRIBUTING HEALTH RISK FACTORS:
Abortion is significantly linked to behavioral changes such as promiscuity, smoking, drug abuse, and eating disorders which all contribute to increased risks of health problems. For example, promiscuity and abortion are each linked to increased rates of PID and ectopic pregnancies. Which contributes most is unclear, but apportionment may be irrelevant if the promiscuity is itself a reaction to post- abortion trauma or loss of self esteem.
INCREASED DANGERS FROM ABORTION FOR TEENAGERS:
Teenagers, who account for about 30 percent of all abortions, are also at much high risk of suffering many abortion related complications. This is true of both immediate complications, and of long-term reproductive damage.14
Psychological Risks Associated with Abortion
REQUIREMENT OF PSYCHOLOGICAL TREATMENT
A study of the medical records of 56,741 California medicaid patients revealed that women who had abortions were 160 percent more likely than delivering women to be hospitalized for psychiatric treatment in the first 90 days following abortion or delivery. Rates of psychiatric treatment remained significantly higher for at least four years.1,3
In a study of post-abortion patients only 8 weeks after their abortion, researchers found that 44% complained of nervous disorders, 36% had experienced sleep disturbances, 31% had regrets about their decision, and 11% had been prescribed psychotropic medicine by their family doctor. (2) A 5 year retrospective study in two Canadian provinces found significantly greater use of medical and psychiatric services among women with a history of abortion. Most significant was the finding that 25% of women who had abortions made visits to psychiatrists as compared to 3% of the control group. (3) Women who have had abortions are significantly more likely than others to subsequently require admission to a psychiatric hospital. At especially high risk are teenagers, separated or divorced women, and women with a history of more than one abortion. (4)
Since many post-abortive women use repression as a coping mechanism, there may be a long period of denial before a woman seeks psychiatric care. These repressed feelings may cause psychosomatic illnesses and psychiatric or behavioral in other areas of her life. As a result, some counselors report that unacknowledged post-abortion distress is the causative factor in many of their female patients, even though their patients have come to them seeking therapy for seemingly unrelated problems. (5)
RISK FACTORS
Researchers have identified a large number of statistically significant risk factors that identify which women are at greatest risk of experiencing one or more severe reactions to abortion. The following is list of risk factors identified by the American Psychological Association Task Force on Mental Health and Abortion in their 2008 report:
- terminating a pregnancy that is wanted or meaningful
- perceived pressure from others to terminate a pregnancy
- perceived opposition to the abortion from partners, family, and/or friends
- lack of perceived social support from others
- various personality traits (e.g., low self-esteem, a pessimistic outlook, low-perceived control over life)
- a history of mental health problems prior to the pregnancy
- feelings of stigma
- perceived need for secrecy
- exposure to antiabortion picketing
- use of avoidance and denial coping strategies
- feelings of commitment to the pregnancy
- ambivalence about the abortion decision
- low perceived ability to cope with the abortion
- history of prior abortion
- late term abortion
- being an adolescent (not an adult)
- having a non-elective (therapeutic or coerced) abortion
- prior history of abortion (having a second or third abortion, or more)
Please see “Identifying High Risk Abortion Patients” or “Abortion decisions and the duty to screen: clinical, ethical, and legal implications of predictive risk factors of post-abortion maladjustment” for a more complete list of risk factors, including citations to the studies identifying each risk factor.
SUICIDAL IDEATION AND SUICIDE ATTEMPTS
Approximately 60 percent of women who experience post-abortion sequelae report suicidal ideation, with 28 percent actually attempting suicide, of which half attempted suicide two or more times.(13) 
Researchers in Finland have identified a strong statistical association between abortion and suicide in a records based study (see figure at the right). They found that the mean annual suicide rate for all women was 11.3 per 100,000 but the rate for women following abortion was 34.7 per 100,000, three times higher. The suicide rate associated with birth, by contrast, was half the rate of all women and less than one-sixth the rate of suicide among women who had abortions.(13)
Suicide attempts appear to be especially prevalent among post-abortion teenagers. Numerous other studies have also revealed higher rates of suicide and suicide attempts associated with abortion.(13)
ALCOHOL AND DRUG ABUSE
Over twenty studies have linked abortion to increased rates of drug and alcohol use.1 Abortion is significantly linked with a two fold increased risk of alcohol abuse among women.(16) Abortion followed by alcohol abuse is linked to violent behavior, divorce or separation, auto accidents, and job loss.(17) In addition to the psycho-social costs of such abuse, drug abuse is linked with increased exposure to HIV/AIDS infections, congenital malformations, and assaultive behavior. (18)
EATING DISORDERS
For at least some women, post-abortion stress is associated with eating disorders such as binge eating, bulimia, and anorexia nervosa. (19)
SEXUAL DYSFUNCTION
Thirty to fifty percent of the women who experience difficulty adjusting to a past abortion report experiencing sexual dysfunctions, of both short and long duration, beginning immediately after their abortions. These problems may include one or more of the following: loss of pleasure from intercourse, increased pain, an aversion to sex and/or males in general, or the development of a promiscuous life-style. (12)
CHILD NEGLECT OR ABUSE
Abortion is linked with increased depression, violent behavior, alcohol and drug abuse, replacement pregnancies, and reduced maternal bonding with children born subsequently. These factors are closely associated with child abuse and would appear to confirm individual clinical assessments linking post-abortion trauma with subsequent child abuse. (20)
POST-TRAUMATIC STRESS DISORDER (PTSD or PAS)
While psychological reactions to abortion fall into many categories, some women experience all or some of they symptoms of post-traumatic stress disorder (PTSD). The lowest incidence rate of PTSD reported following abortion is 1.5%, which would translate to over 600,000 cases of abortion induced PTSD.2 Another study found that 14% of American women have all the symptoms of PTSD and attribute them to their abortions, with as many as 65% reporting some, but not all symptoms of PTSD.3
Yet another random study found that a minimum of 19% of post-abortion women suffer from diagnosable post-traumatic stress disorder (PTSD). Approximately half had many, but not all, symptoms of PTSD, and 20 to 40 percent showed moderate to high levels of stress and avoidance behavior relative to their abortion experiences. (6)
PTSD is a psychological dysfunction which results from a traumatic experience which overwhelms a person’s normal defense mechanisms resulting in intense fear, feelings of helplessness or being trapped, or loss of control. The risk that an experience will be traumatic is increased when the traumatizing event is perceived as including threats of physical injury, sexual violation, or the witnessing of or participation in a violent death. PTSD results when the traumatic event causes the hyperarousal of “flight or fight” defense mechanisms. This hyperarousal causes these defense mechanisms to become disorganized, disconnected from present circumstances, and take on a life of their own resulting in abnormal behavior and major personality disorders. As an example of this disconnection of mental functions, some PTSD victim may experience intense emotion but without clear memory of the event; others may remember every detail but without emotion; still others may reexperience both the event and the emotions in intrusive and overwhelming flashback experiences. (7)
Women may experience abortion as a traumatic event for several reasons. Many are forced into an unwanted abortions by husbands, boyfriends, parents, or others. If the woman has repeatedly been a victim of domineering abuse, such an unwanted abortion may be perceived as the ultimate violation in a life characterized by abuse. Other women, no matter how compelling the reasons they have for seeking an abortion, may still perceive the termination of their pregnancy as the violent killing of their own child. The fear, anxiety, pain, and guilt associated with the procedure are mixed into this perception of grotesque and violent death. Still other women, report that the pain of abortion, inflicted upon them by a masked stranger invading their body, feels identical to rape. (8) Indeed, researchers have found that women with a history of sexual assault may experience greater distress during and after an abortion exactly because of these associations between the two experiences. (9) When the stressor leading to PTSD is abortion, some clinicians refer to this as Post-Abortion Syndrome (PAS).
The major symptoms of PTSD are generally classified under three categories: hyperarousal, intrusion, and constriction.
Hyperarousal is a characteristic of inappropriately and chronically aroused “fight or flight” defense mechanisms. The person is seemingly on permanent alert for threats of danger. Symptoms of hyperarousal include: exaggerated startle responses, anxiety attacks, irritability, outbursts of anger or rage, aggressive behavior, difficulty concentrating, hypervigilence, difficulty falling asleep or staying asleep, or physiological reactions upon exposure to situations that symbolize or resemble an aspect of the traumatic experience (eg. elevated pulse or sweat during a pelvic exam, or upon hearing a vacuum pump sound.)
Intrusion is the reexperience of the traumatic event at unwanted and unexpected times. Symptoms of intrusion in PAS cases include: recurrent and intrusive thoughts about the abortion or aborted child, flashbacks in which the woman momentarily reexperiences an aspect of the abortion experience, nightmares about the abortion or child, or anniversary reactions of intense grief or depression on the due date of the aborted pregnancy or the anniversary date of the abortion.
Constriction is the numbing of emotional resources, or the development of behavioral patterns, so as to avoid stimuli associated with the trauma. It is avoidance behavior; an attempt to deny and avoid negative feelings or people, places, or things which aggravate the negative feelings associated with the trauma. In post-abortion trauma cases, constriction may include: an inability to recall the abortion experience or important parts of it; efforts to avoid activities or situations which may arouse recollections of the abortion; withdrawal from relationships, especially estrangement from those involved in the abortion decision; avoidance of children; efforts to avoid or deny thoughts or feelings about the abortion; restricted range of loving or tender feelings; a sense of a foreshortened future (e.g., does not expect a career, marriage, or children, or a long life.); diminished interest in previously enjoyed activities; drug or alcohol abuse; suicidal thoughts or acts; and other self-destructive tendencies.
As previously mentioned, Barnard’s study identified a 19% rate of PTSD among women who had abortions three to five years previously. But in reality the actual rate is probably higher. Like most post-abortion studies, Barnard’s study was handicapped by a fifty percent drop out rate. Clinical experience has demonstrated that the women least likely to cooperate in post-abortion research are those for whom the abortion caused the most psychological distress. Research has confirmed this insight, demonstrating that the women who refuse followup evaluation most closely match the demographic characteristics of the women who suffer the most post-abortion distress. (10) The extraordinary high rate of refusal to participate in post-abortion studies may interpreted as evidence of constriction or avoidance behavior (not wanting to think about the abortion) which is a major symptom of PTSD.
For many women, the onset or accurate identification of PTSD symptoms may be delayed for several years. (11) Until a PTSD sufferer has received counseling and achieved adequate recovery, PTSD may result in a psychological disability which would prevent an injured abortion patient from bringing action within the normal statutory period. This disability may, therefore, provide grounds for an extended statutory period.
INCREASED SMOKING WITH CORRESPONDENT NEGATIVE HEALTH EFFECTS
Post-abortion stress is linked with increased cigarette smoking. Women who abort are twice as likely to become heavy smokers and suffer the corresponding health risks. (14) Post-abortion women are also more likely to continue smoking during subsequent wanted pregnancies with increased risk of neonatal death or congenital anomalies. (15)
DIVORCE AND CHRONIC RELATIONSHIP PROBLEMS
For most couples, an abortion causes unforeseen problems in their relationship. Post-abortion couples are more likely to divorce or separate. Many post-abortion women develop a greater difficulty forming lasting bonds with a male partner. This may be due to abortion related reactions such as lowered self-esteem, greater distrust of males, sexual dysfunction, substance abuse, and increased levels of depression, anxiety, and volatile anger. Women who have more than one abortion (representing about 45% of all abortions) are more likely to require public assistance, in part because they are also more likely to become single parents. (21)
REPEAT ABORTIONS
Women who have one abortion are at increased risk of having additional abortions in the future. Women with a prior abortion experience are four times more likely to abort a current pregnancy than those with no prior abortion history. (22)
This increased risk is associated with the prior abortion due to lowered self esteem, a conscious or unconscious desire for a replacement pregnancy, and increased sexual activity post-abortion. Subsequent abortions may occur because of conflicted desires to become pregnant and have a child and continued pressures to abort, such as abandonment by the new male partner. Aspects of self-punishment through repeated abortions are also reported. (23)
Approximately 45% of all abortions are now repeat abortions. The risk of falling into a repeat abortion pattern should be discussed with a patient considering her first abortion. Furthermore, since women who have more than one abortion are at a significantly increased risk of suffering physical and psychological sequelae, these heightened risks should be thoroughly discussed with women seeking abortions.
The most complete listing of psychological problems associated with abortion can be found at at AbortionRisks.org
NOTES Regarding Physical Risks
1. Detrimental Effects of Abortion: An Annotated Bibliography with Commentary (Third Edition) is the most complete review of medical studies relevant to abortion. It includes brief summaries of major finding drawn from medical and psychology journal articles, books, and related materials, divided into major categories of relevant injuries. An online version of the bibliography can be found at www.AbortionRisks.com2. Kaunitz, “Causes of Maternal Mortality in the United States,” Obstetrics and Gynecology, 65(5) May 1985.3. H.L. Howe, et al., “Early Abortion and Breast Cancer Risk Among Women Under Age 40,” International Journal of Epidemiology 18(2):300-304 (1989); L.I. Remennick, “Induced Abortion as A Cancer Risk Factor: A Review of Epidemiological Evidence,” Journal of Epidemiological Community Health, (1990); M.C. Pike, “Oral Contraceptive Use and Early Abortion as Risk Factors for Breast Cancer in Young Women,” British Journal of Cancer 43:72 (1981).4. M-G, Le, et al., “Oral Contraceptive Use and Breast or Cervical Cancer: Preliminary Results of a French Case- Control Study, Hormones and Sexual Factors in Human Cancer Etiology, ed. JP Wolff, et al., Excerpta Medica: New York (1984) pp.139-147; F. Parazzini, et al., “Reproductive Factors and the Risk of Invasive and Intraepithelial Cervical Neoplasia,” British Journal of Cancer, 59:805-809 (1989); H.L. Stewart, et al., “Epidemiology of Cancers of the Uterine Cervix and Corpus, Breast and Ovary in Israel and New York City,” Journal of the National Cancer Institute 37(1):1-96; I. Fujimoto, et al., “Epidemiologic Study of Carcinoma in Situ of the Cervix,” Journal of Reproductive Medicine 30(7):535 (July 1985); N. Weiss, “Events of Reproductive Life and the Incidence of Epithelial Ovarian Cancer,” Am. J. of Epidemiology, 117(2):128-139 (1983); V. Beral, et al., “Does Pregnancy Protect Against Ovarian Cancer,” The Lancet, May 20, 1978, pp. 1083-1087; C. LaVecchia, et al., “Reproductive Factors and the Risk of Hepatocellular Carcinoma in Women,” International Journal of Cancer, 52:351, 1992.
5. S. Kaali, et al., “The Frequency and Management of Uterine Perforations During First-Trimester Abortions,” Am. J. Obstetrics and Gynecology 161:406-408, August 1989; M. White, “A Case-Control Study of Uterine Perforations documented at Laparoscopy,” Am. J. Obstetrics and Gynecology 129:623 (1977).
6. D. Grimes, et al., “Prevention of uterine perforation During Curettage Abortion,” JAMA, 251:2108-2111 (1984); D. Grimes, et al.,”Local versus General Anesthesia: Which is Safer For Performing Suction Abortions?” Am. J. of Obstetrics and Gynecology, 135:1030 (1979).
7. K. Schulz, et al., “Measures to Prevent Cervical Injuries During Suction Curettage Abortion,” The Lancet, May 28, 1983, pp 1182-1184; W. Cates, “The Risks Associated with Teenage Abortion,” New England Journal of Medicine, 309(11):612-624; R. Castadot, “Pregnancy Termination: Techniques, Risks, and Complications and Their Management,” Fertility and Sterility, 45(1):5-16 (1986).
8. Barrett, et al., “Induced Abortion: A Risk Factor for Placenta Previa”, American Journal of Ob&Gyn. 141:7 (1981).
9. Hogue, Cates and Tietze, “Impact of Vacuum Aspiration Abortion on Future Childbearing: A Review”, Family Planning Perspectives (May-June 1983),vol.15, no.3.. Jacobsson B, Hagberg G, Hagberg B, Ladfors L, Niklasson A, Hagberg A. Cerebral Palsy in preterm infants: a population-based case-control study of antenatal and intrapartal risk factors. Acta Paediatrica 2002;91:946-951. Calhoun BC, Shadigian E, Rooney B. Cost consequences of induced abortion as an attributable risk for preterm birth and informed consent. J Reprod Med 2007;52:929-939.
10. Daling,et.al., “Ectopic Pregnancy in Relation to Previous Induced Abortion”, JAMA, 253(7):1005-1008 (Feb. 15, 1985); Levin, et.al., “Ectopic Pregnancy and Prior Induced Abortion”, American Journal of Public Health (1982), vol.72,p253; C.S. Chung, “Induced Abortion and Ectopic Pregnancy in Subsequent Pregnancies,” American Journal of Epidemiology 115(6):879-887 (1982)
11. T. Radberg, et al., “Chlamydia Trachomatis in Relation to Infections Following First Trimester Abortions,” Acta Obstricia Gynoecological (Supp. 93), 54:478 (1980); L. Westergaard, “Significance of Cervical Chlamydia Trachomatis Infection in Post-abortal Pelvic Inflammatory Disease,” Obstetrics and Gynecology, 60(3):322-325, (1982); M. Chacko, et al., “Chlamydia Trachomatosis Infection in Sexually Active Adolescents: Prevalence and Risk Factors,” Pediatrics, 73(6), (1984); M. Barbacci, et al., “Post- Abortal Endometritis and Isolation of Chlamydia Trachomatis,” Obstetrics and Gynecology 68(5):668-690, (1986); S. Duthrie, et al., “Morbidity After Termination of Pregnancy in First-Trimester,” Genitourinary Medicine 63(3):182-187, (1987).
12. Burkman, et al., “Morbidity Risk Among Young Adolescents Undergoing Elective Abortion” Contraception, 30:99-105 (1984); “Post-Abortal Endometritis and Isolation of Chlamydia Trachomatis,” Obstetrics and Gynecology 68(5):668- 690, (1986)
13. Frank, et.al., “Induced Abortion Operations and Their Early Sequelae”, Journal of the Royal College of General Practitioners (April 1985),35(73):175-180; Grimes DA, Cates W Jr. Abortion: Methods and complications. In: Hafez ESE, ed. Human reproduction: Conception and contraception (2nd ed). Hagerstown, Maryland: Harper and Row, 1980:796‑813.; M.A. Freedman, “Comparison of complication rates in first trimester abortions performed by physician assistants and physicians,” Am. J. Public Health, 76(5):550- 554 (1986).
14. Wadhera, “Legal Abortion Among Teens, 1974-1978”, Canadian Medical Association Journal, 122:1386-1389,(June 1980).
15. Ney, et.al., “The Effects of Pregnancy Loss on Women’s Health,” Soc. Sci. Med. 48(9):1193-1200, 1994; Badgley, Caron, & Powell, Report of the Committee on the Operation of the Abortion Law, Supply and Services, Ottawa, 1977: 319-321.
16. Gissler, M., et. al., “Pregnancy-associated deaths in Finland 1987-1994 — definition problems and benefits of record linkage,” Acta Obsetricia et Gynecolgica Scandinavica 76:651-657 (1997).
17. Zhou, Weijin, et. al., “Induced Abortion and Subsequent Pregnancy Duration,” Obstetrics & Gynecology 94(6):948-953 (Dec. 1999). Klemetti R, Gissler M, Niinimäki M, Hemminki E. Birth outcomes after induced abortion: a nationwide register-based study of first births in Finland. Hum Reprod 2012 Aug 29. [Epub ahead of print]. Rooney B, Calhoun BC. Induced Abortion and Risk of Later Premature Births. Journal American Physicians & Surgeons 2003;8(2):46-49 Bhattacharya S, Lowit A, Bhattacharya S, Raja EA. -et al. Reproductive outcomes following induced abortion: a national register-based study in Scotland. BMJ OPEN Summer 2012. Swingle HM, Colaizy TT, Zimmerman MB, et al Abortion and the risk of subsequent preterm birth: a systematic review and meta-analysis. J Reproductive Med 2009;54:95-108.
18. D. Berkeley, P.L. Humphreys, and D. Davidson, “Demands Made on General Practice by Women Before and After an Abortion,” J. R. Coll. Gen. Pract. 34:310-315, 1984.
19. Frank, et.al., “Induced Abortion Operations and Their Early Sequelae”, Journal of the Royal College of General Practitioners (April 1985), vol.35,no.73,pp175-180. and Grimes and Cates, “Abortion: Methods and Complications”, Human Reproduction, 2nd ed., 796-813.
NOTES RELATIVE TO SECTION ON PSYCHOLOGICAL RISKS:
1. An excellent resource is Thomas Strahan’s Detrimental Effects of Abortion: An Annotated Bibliography with Commentary (Third Edition) This resource includes brief summaries of major finding drawn from medical and psychology journal articles, books, and related materials, divided into major categories of relevant injuries. An online version can be found at AbortionRisks.org
2. Ashton,”They Psychosocial Outcome of Induced Abortion”, British Journal of Ob&Gyn., 87:1115-1122, (1980).
3. Badgley, et.al.,Report of the Committee on the Operation of the Abortion Law (Ottawa:Supply and Services, 1977)pp.313-321.
4. R. Somers, “Risk of Admission to Psychiatric Institutions Among Danish Women who Experienced Induced Abortion: An Analysis on National Record Linkage,” Dissertation Abstracts International, Public Health 2621-B, Order No. 7926066 (1979); H. David, et al., “Postpartum and Postabortion Psychotic Reactions,” Family Planning Perspectives 13:88-91 (1981).
5. Kent, et al., “Bereavement in Post-Abortive Women: A Clinical Report”, World Journal of Psychosynthesis (Autumn-Winter 1981), vol.13,nos.3-4.
6. Catherine Barnard, The Long-Term Psychological Effects of Abortion, Portsmouth, N.H.: Institute for Pregnancy Loss, 1990).
7. Herman, Trauma and Recovery, (New York: Basic Books, 1992) 34.
8. Francke, The Ambivalence of Abortion (New York: Random House, 1978) 84-95.
9. Zakus, “Adolescent Abortion Option,” Social Work in Health Care, 12(4):87 (1987); Makhorn, “Sexual Assault & Pregnancy,” New Perspectives on Human Abortion, Mall & Watts, eds., (Washington, D.C.: University Publications of America, 1981).
10. Adler, “Sample Attrition in Studies of Psycho-social Sequelae of Abortion: How great a problem.” Journal of Social Issues, 1979, 35, 100-110.
11. Speckhard, “Postabortion Syndrome: An Emerging Public Health Concern,” Journal of Social Issues, 48(3):95-119.
12. Speckhard, Psycho-social Stress Following Abortion, Sheed & Ward, Kansas City: MO, 1987; and Belsey, et al., “Predictive Factors in Emotional Response to Abortion: King’s Termination Study – IV,” Soc. Sci. & Med., 11:71-82 (1977).
13. Speckhard, Psycho-social Stress Following Abortion, Sheed & Ward, Kansas City: MO, 1987; Gissler, Hemminki & Lonnqvist, “Suicides after pregnancy in Finland, 1987-94: register linkage study,” British Journal of Medicine 313:1431-4, 1996.C. Haignere, et al., “HIV/AIDS Prevention and Multiple Risk Behaviors of Gay Male and Runaway Adolescents,” Sixth International Conference on AIDS: San Francisco, June 1990; N. Campbell, et al., “Abortion in Adolescence,” Adolescence, 23(92):813-823 (1988); H. Vaughan, Canonical Variates of Post-Abortion Syndrome, Portsmouth, NH: Institute for Pregnancy Loss, 1991; B. Garfinkel, “Stress, Depression and Suicide: A Study of Adolescents in Minnesota,” Responding to High Risk Youth, Minnesota Extension Service, University of Minnesota (1986).
14. Harlap, “Characteristics of Pregnant Women Reporting Previous Induced Abortions,” Bulletin World Health Organization, 52:149 (1975); N. Meirik, “Outcome of First Delivery After 2nd Trimester Two Stage Induced Abortion: A Controlled Cohort Study,” Acta Obsetricia et Gynecologica Scandinavia 63(1):45-50(1984); Levin, et al., “Association of Induced Abortion with Subsequent Pregnancy Loss,” JAMA, 243:2495-2499, June 27, 1980.
15. Obel, “Pregnancy Complications Following Legally Induced Abortion: An Analysis of the Population with Special Reference to Prematurity,” Danish Medical Bulletin, 26:192- 199 (1979); Martin, “An Overview: Maternal Nicotine and Caffeine Consumption and Offspring Outcome,” Neurobehavioral Toxicology and Tertology, 4(4):421-427, (1982).
16. Klassen, “Sexual Experience and Drinking Among Women in a U.S. National Survey,” Archives of Sexual Behavior, 15(5):363-39 ; M. Plant, Women, Drinking and Pregnancy, Tavistock Pub, London (1985); Kuzma & Kissinger, “Patterns of Alcohol and Cigarette Use in Pregnancy,” Neurobehavioral Toxicology and Terotology, 3:211-221 (1981).
17. Morrissey, et al., “Stressful Life Events and Alcohol Problems Among Women Seen at a Detoxification Center,” Journal of Studies on Alcohol, 39(9):1159 (1978).
18. Oro, et al., “Perinatal Cocaine and Methamphetamine Exposure Maternal and Neo-Natal Correlates,” J. Pediatrics, 111:571- 578 (1978); D.A. Frank, et al., “Cocaine Use During Pregnancy Prevalence and Correlates,” Pediatrics, 82(6):888 (1988); H. Amaro, et al., “Drug Use Among Adolescent Mothers: Profile of Risk,” Pediatrics 84:144-150, (1989)
19. Speckhard, Psycho-social Stress Following Abortion, Sheed & Ward, Kansas City: MO, 1987; J. Spaulding, et al, “Psychoses Following Therapeutic Abortion, Am. J. of Psychiatry 125(3):364 (1978); R.K. McAll, et al., “Ritual Mourning in Anorexia Nervosa,” The Lancet, August 16, 1980, p. 368.
20. Benedict, et al., “Maternal Perinatal Risk Factors and Child Abuse,” Child Abuse and Neglect, 9:217-224 (1985); P.G. Ney, “Relationship between Abortion and Child Abuse,” Canadian Journal of Psychiatry, 24:610-620, 1979; Reardon, Aborted Women – Silent No More (Chicago: Loyola University Press, 1987), 129-30, describes a case of woman who beat her three year old son to death shortly after an abortion which triggered a “psychotic episode” of grief, guilt, and misplaced anger.
21. Shepard, et al., “Contraceptive Practice and Repeat Induced Abortion: An Epidemiological Investigation,” J. Biosocial Science, 11:289-302 (1979); M. Bracken, “First and Repeated Abortions: A Study of Decision-Making and Delay,” J. Biosocial Science, 7:473-491 (1975); S. Henshaw, “The Characteristics and Prior Contraceptive Use of U.S. Abortion Patients,” Family Planning Perspectives, 20(4):158-168 (1988); D. Sherman, et al., “The Abortion Experience in Private Practice,” Women and Loss: Psychobiological Perspectives, ed. W.F. Finn, et al., (New York: Praeger Publ. 1985), pp98-107; E.M. Belsey, et al., “Predictive Factors in Emotional Response to Abortion: King’s Termination Study – IV,” Social Science and Medicine, 11:71- 82 (1977); E. Freeman, et al., “Emotional Distress Patterns Among Women Having First or Repeat Abortions,” Obstetrics and Gynecology, 55(5):630-636 (1980); C. Berger, et al., “Repeat Abortion: Is it a Problem?” Family Planning Perspectives 16(2):70-75 (1984).
22. Joyce, “The Social and Economic Correlates of Pregnancy Resolution Among Adolescents in New York by Race and Ethnicity: A Multivariate Analysis,” Am. J. of Public Health, 78(6):626-631 (1988); C. Tietze, “Repeat Abortions – Why More?” Family Planning Perspectives 10(5):286-288, (1978).
23. Leach, “The Repeat Abortion Patient,” Family Planning Perspectives, 9(1):37-39 (1977); S. Fischer, “Reflection on Repeated Abortions: The meanings and motivations,” Journal of Social Work Practice 2(2):70-87 (1986); B. Howe, et al., “Repeat Abortion, Blaming the Victims,” Am. J. of Public Health, 69(12):1242-1246, (1979).
Abortion Risks and Complications, copyright 1997, 2000 Elliot Institute.



Hey guys l need help, my mother had several abortion. Abort 15 to 20 year and l would like to know the effects on her and me……
The most likely impact on your mother is unresolved grief. I’d suggest you take a look at our summary page on the psychological effects of abortion and the risk factors that predict more emotional problems with a past abortion. If she is open to it, she may benefit from talking to other women who have been through the healing process after an abortion loss.
In regard to any impact on you, I think it is most likely that you could be impacted by emotional effects on her that may have affected the way she parented you or bonded with you. In some cases, children who are aware of or sense an abortion loss may also have their own unresolved feelings of loss regarding a sibling, or siblings, and also a form of “survivor” syndrome, characterized by angst over “Why did I survive? What if it had been me?” Here is a link to a page of studies that may have some bearing on the impact of abortion on siblings and on marriages and parenting.
After reading the links above, please let me know if you have more questions.
hello am mueni third year student .I’m 2 months pregnant but I don’t have peace because of several issues …I don’t trust my boyfriend because he likes chatting with many women secondly my parents are very tough they can decide not to pay my school fees..
I want to abort but my boyfriend is against it ..
please help me
Hi Triza,
Have you looked at the risk factors that predict more problems after an abortion?
I would suggest you go through that list carefully. From even the little you have told me, I think it highly likely you would someday come to regret your abortion and suffer great grief.
I realize that it is hard to see how things can work out if you give birth to your child, but trust me, they will. You may also be surprised (I hope) by your parents being more understanding and supportive than you imagine.
Your boyfriend is willing to stand beside you and to be a good father to your baby. Give him a chance.
You are in my prayers.
I had an abortion last month and since then have being seen blood,sometimes clothed one,sometimes ordinary stains,the blood has now turn to slightly tick and dark color now.pls what shld I do.
Hi Temitope,
If you think you are having complications or something doesn’t seem right, you should definitely see a doctor. If it seems serious I would not go back to the abortion clinic but would seek out another doctor at a medical office or hospital. And definitely tell the doctor that you recently underwent an induced abortion so he or she will know how best to treat your symptoms if you do need medical care.
I don’t know your circumstances, but if you are struggling emotionally at all, you can visit our healing page for information and resources that can help. There are organizations listed there that offer emotional and spiritual support to help you heal, or just a listening ear if you need to talk. If you aren’t ready to make a phone call but still want help, Rachel’s Vineyard offers support through email as well as a Q&A forum where you can ask questions about healing, etc. You can also contact OptionLine for post-abortion support through LiveChat or text (text “HELPLINE” to 313131).
I forgot to add, if you live in the US and need help finding a doctor who can help, visit here for more information: http://aaplog.org/
Hi good evening am really in a confused stage right now am a month pregnant and it seems the owner is not interested what should I do?
There are a lot of people and groups who can assist you with emotional and financial support to help you with your child. Here is one place to look for a list of groups offering help near to you.
As you can see from the list of risks associated with abortion, we strongly discourage that option.
If you give us more details regarding the city where you live, perhaps we can help find a pregnancy help center that can help you.
You are in my prayers, Ruth.
Don’t give into despair. Things will work out. Open your mind and heart to the love and help of the people who do want to stand by you. Preferably, that should come from the child’s father and both your and his family. If it does not, there are many who will step in to give you the support that they don’t.
I had 5 abortions within 3 years.2013-2015.I was so depressed and unhappy for a very long time.No one knew,even my mother! Then I met a pastor who I was finally able to open up,i confessed everything for the first time and we prayed together for Mercy and Restoration and truly I felt free and no longer burdened with pain and guilt . till date,tho I’m in my early 20s and unmarried,i hvnt had another abortion and I truly feel no guilt.I don’t know what the future holds but I’m very positive. & if your dealing with regrets,guilt and fear of the future, I hope you find Jesus.Its true!theres something about casting ur burdens on him and you’ll feel whole again and face the future excitingly.
I am so glad you found so much peace and healing. You are in our prayers. And I pray you will keep us and our work in your prayers as we seek to share that same peace and healing with others.
I have done 7 times abortion and I’m pregnant again. I really don’t know what to do.my boyfriend and me are no more. Please is there any negative effect of many abortion? Thank you
Hello Nadia, I’m so glad you found our site. I don’t know your circumstances, or what has led you to the situation you are currently in or to your past abortions. But please know that whatever is going on in your life, you don’t have to continue this cycle. It may seem like you don’t have any other choices, especially if the baby’s father is no longer in the picture. But you do have options and with the right help, you can protect the baby growing inside of you and make good choices for yourself and your unborn child.
Right now you are likely in crisis — perhaps you feel like you aren’t ready to have a baby or are worried about what this means for your future. Maybe you are facing the prospect of having a child alone, or even being pushed, pressured or forced by others to have an abortion. Perhaps you believe that having an abortion is your only option. It’s okay to be scared or to feel whatever it is you are feeling. But what you shouldn’t do is let those worries and any difficulties you are having right now drive you to make a decision you might regret. Abortion is a decision you can’t undo, and it’s hard to make good decisions when you are facing a crisis.
The fact that you are coming to this site and asking questions about the risks leads me to think that you are having doubts about undergoing another abortion. I can’t give you any advice on your medical health, but studies have found that repeat abortions do carry risks, including a higher risk of maternal death, breast cancer, preterm birth in later pregnancies, and higher psychological risks for the mother. Plus, abortions in general have all kinds of physical and psychological risks attached to them. So yes, you could be putting yourself at risk by having repeat abortions.
If you have concerns about your physical or mental health due to the abortions you’ve had, you should talk to a doctor or counselor. If you live in the US and don’t have a doctor already that you trust to talk with about this, you might consider contacting the American Association of Pro-Life Ob/Gyns. They won’t be able to diagnose any problems from a distance, but they might be able to give you some information to put you at ease or put you in touch with a doctor who can help. They may be able to help you with your medical needs during this current pregnancy as well, so please contact them if you don’t have a doctor!
Second, there are many organizations out there that support women during and after pregnancy, and who can help you sort your plans. This page has a list of organizations nationwide who offer options counseling, practical support (such as medical, housing, school, job, etc) and more to women who are pregnant. You can also get help from OptionLine by texting HELPLINE to 313131 or through their Live Chat link. If you are outside the U.S., contact us at elliotinstitute@gmail.com and I will try to find a local organization that can help you.
Another thing a pregnancy center can help you with is post-abortion counseling. Even if you don’t feel like your past abortions are affecting things for you, you may have unresolved grief or pain that is driving you to have repeat abortions or affecting other areas of your life. There are groups that offer free and confidential support to help work through these issues and free you from any past issues that are affecting you. They would love to talk with you even if you just call to ask some questions. If you are looking for advice this is a great place to start.
You need to listen to your heart, find people who can support you and get real information about your options — and you do have options even though it might feel like you don’t. Don’t let yourself be pushed into making a hasty decision you might regret. I would really, really encourage you to look into ALL your options — you need to make sure you have all the information possible before making such a life-altering decision.
Feel free to send us an email if you need more information or to be put in touch with a group that can help you: elliotinstitute@gmail.com
please remember that a child is a gift from God so do not kill your gift someone is looking for it now but nothing is happening now, I encourage to keep that blessing and God will give you another way to look after it. 1 day that baby will happy to see the stars and the nice colours of the world
I have so much trauma from abortion. If you are not in a position to parent your child, you can gift her to someone in adoption. You will be negatively impacted by the pain of abortion for life. Find a pregnancy resource center and ask for assistance. Many people will love you through this.
Dear Palesa,
Please don’t give up on your CHILD. If you do, who else will protect him/her? You are a MOTHER already!
Please, visit http://www.bravelove.org to see what other women have done for their children. You will be amazed by their stories and will find courage to be a great, courageous and brave mother yourself.
God bless you and your child forever!!!
Maria Katerina from Albania
Dear Palesa,
I was saddened to hear of your situation and your distress, which is so understandable.
I am in Melbourne, Australia, so there’s little I can do to help you directly. But I am a priest and I want you to know that I am praying for you and your baby, and will offer the Holy Mass for you both this evening.
Know that people here in Australia are praying for you, and in other parts of the world. You are not alone.
Peace and grace,
Father Robin
It sounds like you love your baby already and care for her or him. One answer you might consider is adoption. Open adoption can give you some control as to who adopts your baby. We know someone who adopted this way and stays in touch with the birth mother. You would be a very loving mother in choosing adoption if you are not resdy to raise a child right now
Palesa, I have been praying for you and your baby. Thank you for reaching out.
I was not that smart when I was thinking of having an abortion and ‘leaning on my own understanding’, had the abortion.
It was the worst, most horrific thing I have ever done in my life. It never really leaves me, the memory cannot be wiped out, the deed cannot be undone. It is so very final.
I beg you on behalf of your unborn child, ” Please Mommy, let me live. I want to see your face, your smile, feel your arms holding me,,,,now all I hear is your voice and your words and your worries,and I am scared that you will not love me enough to keep me. Please love yourself as much as I love you because with my death you would be killing a part of yourself and the repercussions will never leave you. Please don’t worry about Grandma she will love me as soon as she sees me, how can she help it, she loves you and wants what is best for you and I am a part of you. Please Mommy please, choose life for us.”
Only God can create life. Your baby is a gift from Him. He sees the bigger picture, we only see a little part of it. Only He knows why this child was sent to you now.
Get a Bible, get on your knees, read, pray, get to know your Father and Creator, talk to Him. With God all things are possible. He does not force himself on us, He has given us ‘free will’, we have to humbly ask for His help if we want it.
All the choices are yours.
God Bless you and your baby abundantly. May God grant you wisdom and understanding in this matter.
Dear Palesa,
I am praying for you that you will embrace life and be a life-giver, as it appears you do want to be. Nurturing and respecting life is always better in the long run for your body and soul and there are options as so many people have already indicated. Your baby is already a unique living little person. Please give that child the great gift of the chance to be born and to know and love you. Another loving option is that of allowing another couple the opportunity to know and love this child if you feel you really are not able to care for the child right now. Aside from these reasons to bring your pregnancy to fruition, there are many health reasons for you to consider, too. Continue the courageous path you have already started down by reaching out for help and looking at this website. Check out the resource suggestions. There are many people out there who want to help you and who understand. You and your child will remain in my prayers dear Palesa. . Go bless you.
I’m pregnant for man I thought I love, he’s interested in me via marriage. I’m 4 months now he’s not showing concern and I’m feeling terribly bad I don’t want abortion but my family is against me now I’m very ashamed of myself and for DAT I can’t do anything. I feel so worthless what can I do
Dear Dequeen,
I understand how overwhelmed you feel. But please, don’t give into the pressure to abort. The dangers are very real. But most certain of all is that if you had an abortion you would regret it the rest of your life.
Read some of the comments in response to a very similar message just posted on the same page by a 17-year-old Palesa.
There are so many women who have been exactly in the same spot as you and Palesa who are encouraging you to make a better chioce. Choose life. As one woman commented: Abortion stops one heart and breaks a second. It will only break your heart.
If your man or family push for an abortion, tell them first to read about the physical and emotional effects of abortion. How can they really want you to go through that?
Also, please read about the risk factors that identify women at greatest risk, as it is likely that you fit into one or more of these higher risk categories.
Please keep in touch. Let us know how you are doing. You’re in my prayers.
Dear Palesa,
I was also in your situation at age 17 and thinking I had made a terrible mistake getting pregnant. I chose an abortion. To this day ( I am now 63 ) I miss that child and the life I might have had if I had not made the choice I did. I have never married or had children.
Please this is a decision that will effect the rest of your life. God is on the side of life. Trust Him to help you and guide you and you will be rewarded beyond measure. I will be praying for you.
Dear Palesa,,
I understand how you must be feeling. This is your little baby who is depending on you to protect it. This little one’s heart is beating under your heart.
Don’t make the same mistake that I did. I was just a little bit older than you when I got pregnant and I was very confused and had no one to support me and out of fear I aborted my baby. I suffered for years from such pain and grief.
I would give my life to have my child back. Please allow people to help you to give life to your child and if you feel you cannot support your child you could make an adoption plan.
Abortion stops one heart and breaks another. I am praying for you.
I will be praying for you, Palesa. (You have such a beautiful name!) I know the fear and confusion you’re feeling now. I was just a year older than you when I became pregnant 38 years ago. My boyfriend wanted me to have an abortion, and I even made an appointment to have one. But, I am eternally grateful that I did not have that abortion and instead chose to allow my child to live.
During the pregnancy, I considered adoption (which is a beautiful choice – one that blesses the mother, the child, and the adopting family!), but I decided to raise him myself even though I was going to be a single mother. As it turned out, I was able to continue my education and get my Masters degree. I have never once regretted my decision. My son is one of the most loving, kind, and thoughtful human beings I know. I shudder to think of how close I came to never knowing him, all because of fear.
I encourage you to look into open adoption if you feel you are not yet ready to continue being a Mom. (I say “continue” because you already are a Mom, since your little one is safe inside your womb;-)
I will pray that joy replace fear about your pregnancy!
Dear Palesa, I am praying for you and your Baby.
Your Baby is not a mistake. God call him/her to be for a purpose. Trust God!
Dear Palesa, you are not alone in this. God will give you all the graces necessary if you choose life for you and your child. You are already a Mom. I’ve been working with people who have suffered the aftermath of abortion for 13 years and I want more for you and your child than what they have had to live with. Please contact your local crisis pregnancy center. There is help for both of you now and after the birth of your child. There may be times of difficulty, but you won’t have the mental anguish of denying your child life. I am praying for all of you Palesa… please choose life so you both may live.
Dear Palesa:
I have a close friend who gave her baby up for adoption 51 years ago. This mother’s day they were reconnected thanks to a DNA search through Ancestor.com. It turns out a wonderful family adopted her, and she went on to get a bachelor’s and then a master’s degree, and is now halfway through work on her PhD. What a loss it would have been to both of them and to the world if she had been aborted. I know of others where similar outcomes have come from having their babies instead of aborting them; but I know of no woman who aborted who is happy about that decision today. Many never recover. Take the long view, and reach out to those who have offered to help. Your own eternal happiness is at stake.
I pray for you. Palesa and for your baby and for your boy friend and all others involved in your situation. May God turn this difficulty into a triumph of his grace. You can meet this challenge and having done so you will be a better, stronger person.Troubles overcome build character. you will never regret cherishing this new life within you, a life that comes from the hand of God. Rise up for Jesus who suffered much for us purely out of love Take the long term view. All things pass. God remains. Let me know what I can do to help you and your baby, God’s gift to you and all his people/
We ask our Dear Lord to create an urgent and positive supportive response to this Dear Mom and the Young Man, now the Dad, who together need to be support victims for the lives of creative beings within their lives together. Are You reading this Dear Lord? Peace!
Palesa, I am praying for you. I understand your feelings. When I was 17 I became pregnant. My family was not supportive at all to me. My parents took me to have an abortion. There is not a day that goes by that my heart does not long for my child. There are so many resources avIlable to you today that were not there for me. First contact your local pregnancy center. Then look to see what other resources are in your area. Reaearxh to see if an organization called Embrace Grace is in your area. Embrace Grace is usually in a local church body and will walk along side of you during and after your pregnancy. Prayers for the Father to open doors of opportunity for you.
Dear Palesa,
I am praying for you in Poland. I will tell friends about your situation. I have many adopted people in my family; some of my friends have adopted children; and I know a young couple who cannot have children, and are so loving and so much want children. They are going to start the process to become adoptive parents this autumn.
There are so many loving hearts in the world who would raise your baby in a happy, safe and warm home! But there is only ONE heart that your baby is relying on right now, and that is YOUR heart.
Your baby is depending on YOU. Your baby has only YOU. If your baby could speak now, your baby would ask you, ‘Mom, please let me live; please let me look you in the eyes; please, let me love you; please let me grow up.’
You can say ‘Yes’ to your baby by keeping her or by giving her to a loving couple for adoption.
Your baby is depending on YOU and only you to protect her from harm and see her safely into the world. It is a lot to ask of a 17-year-old, but your baby doesn’t know you are 17 and a learner. Your baby only knows that she is inside you, under your heart, safe and protected, and that you are her mother.
Palesa, you will love this baby more than anything! And so will your family. Take advantage of all of the help that is available. I am praying for you!
Dear Palesa,
You already are a mother! Since the day of conception you have been the mother of this gift from God. Please find a pregnancy resource center near you. They will help support you through this hard time and help you provide for this baby if you decide to parent, or help you with an adoption plan if you decide you can’t at this time. Know that you have the prayer support of many and you can make it through this in a way that will give you peace.
Dear Palesa,
I am very sorry for your pain.
I work in Project Rachel Ministry. It helps women and men who are suffering from an abortion decision. When I listen to their stories, my heart is so filled with sorrow. I can understand why they thought that abortion was the answer at that moment but they found out so many things after the abortion that they did not know before. Not one of them would have chosen abortion if they had know all the pain that they would feel. Some feel regret during the abortion, some right after, and some bury it deep in their heart for years.
When I am facing a difficult decision, I often imagine my life five years from now looking back at this moment. I also think about other times in my life when I made an important decision and see how it changed my life. It helps me to know that I can get through hard times because I have done it before.
There are lots of people who care and will help you. Abortion is forever. Please do what the person who wrote the last message said about reading testimonies of other teens facing an unplanned pregnancy. You will probably be able to see yourself in their stories.
You are worth it Palesa, so is your baby.
Sincerely,
Allison
Please finish your pregnancy. It is better for you and all. You have months ahead to look at all the options for care. With abortion, you will have a lifetime of regret. Not worth it!
Hello, I know many who would gladly adopt your baby. Please keep the child and trust God to work all things out. I am praying for you right now. No one should ever force you to remove a child from the safety of your womb. You have already shown great courage in contacting other for help and prayer. You are loved greatly.
I am one of many who are praying for you, Palesa. Adoption is a loving option and open adoption means that you can write letters to your child and get reports and pictures from the adoptive parents. Parenting is also a possibility and as someone has already said, we are never ready! I was the youngest of my family and had little experience with young children but a parenting class helped a lot and I just kept praying for God to help me be a good Mom. So many women so deeply regret their abortions; I am praying you will give your child life. You will have months to decide between adoption and parenting.
Palesa, open your heart to the help that so many are standing by ready to give you. Open your heart to your baby. There is no one like him or her in the universe and never will be again. And YOU are the perfect mother chosen to bring this one-in-the-universe child into this world.
Believe in yourself… so many others do and God our loving Father believes in you too.
Dear Palesa,
Sweetheart, adoption is one of the truest expressions of the selfless love of a mother who wants the best for her child. There are 1.4 Million couples waiting to adopt a baby just here in the U.S.. Most of these couples are unable to have a baby on their own and would pay for all of your medical expenses and more. I know a woman who experienced both abortion and adoption who said this: “I look back at the 3 babies I no longer have, but with very different feelings. The 2 that I aborted fill me with grief and regret, but when I think of the one I placed for adoption I’m filled with joy because I know he is being raised by a family that wanted him desperately, loves him and is providing everything he needs to be all he can be.”
I befriended a girl several months ago and she is choosing adoption and sees it as what God intended all along for her. Her employer and many people God has since put in her path is an incredible witness to that fact.
Most agencies will provide counseling for you, coverage for your medical care, and allow you to choose a family for your child. In an open adoption you may be able to keep in touch with your child and interact and see how their life progresses.
I have many friends who have been waiting years to adopt. The most beautiful and loving couples that you could possibly imagine but they have had one miscarriage after another. They would give your baby so much love and everything she needs to fulfill her destiny. Every child is sent into this world by God with a unique message to deliver, a new song to sing and many personal acts of love to bestow. If you explore the Elliot Institutes resources on adoption you will be able to find links to many adoption ministries and agencies where you can view literally thousands of couple’s profiles who have been approved and passed all the requirements to adopt.
I want to share a personal story with you. I was reading an article that was talking about how many pregnancy centers, when telling women about how adoption is a viable option women will say “What kind of a mother would I be to put my baby up for adoption so would choose to abort instead. As I read these words a story in the Bible just started flashing and flashing and wouldn’t stop. I had to search for it and when I did I had to read it a couple times to really grasp the power of what it said. I was familiar with it but always thought it was merely speaking of the wisdom of Solomon and not a lesson about adoption. Two women had babies at the same time. One of them rolled over in her sleep and smothered her baby. Then she switched babies and it was up to Solomon to determine who the true mother was. “Then Solomon said “This woman says that it is my child who is living and yours is the dead one, but the other woman says NO! Yours is the dead one and the living child belongs to me! So the King said “Bring me a sword!” So a sword was brought before the King and he said “Divide the living child in two, Give half to the one and half to the other! But the woman who’s child was living’s heart yearned with compassion for her son so she spoke to the King and said “O my Lord, Give HER the living child and BY NO MEANS harm him, but the other woman said “Let him be neither mine or yours but divide him!” Sweetheart some loving and incredibly strong mothers love their child so much that they would let them go to another rather than allow any harm come to them. These two women represent these two opposite mindsets of a woman who would place her child for adoption and the woman who would say “What kind of a mother would I be to put my child up for adoption” and would instead choose abortion. “Let him be neither mine nor hers but divide him.”
I just produced a documentary where we interviewed many loving and caring mothers who placed their children and have open adoptions where they get to see their child grow up and participate in their life. They in effect make another couples dream come true. It is a beautiful situation that allows a mother to not have to live with the guilt and regret of an abortion decision. conceivedinrape.com
Honey adoption is a win win course of action. The baby wins because its life is preserved into a loving, providing home. The adoptive parents win because you provided them a baby that nature wouldn’t let them have on their own. You win because you embrace your identity as a mother by choosing whats best for your child. Time and again Ive heard parents who adopted children say that they are certain that the child they adopted was the child God wanted them to have all along!!! Think about how beautiful and profound that is. It means that the biological mother embraced her divinely appointed destiny by providing the very child that God intended the adoptive parents to have. Perhaps from before time began! Isn’t that beautiful?
God DELIGHTS to help women in crisis pregnancies! His Own Mother was in a crisis pregnancy. He LOVES adoption too. Jesus said “I will not leave you orphans, I will come for you.” To children who are adopted Jesus looks a whole lot like Mom and Dad. 😉 I know a girl who was adopted along with another girl because the adoptive parents were unable to have a baby on their own. Fifteen years later guess what? They had their own biological child. My friend and her sister would tease him. Mom and Dad “Had” you but they “Chose” us! 😉
Sweetheart, oftentimes God will send someone into our lives to help us, to rescue us, to break our chains and set us free. Most often that person is a child. I can read your hurt and pain at the thought of aborting this child. Your pain is so palpable that I can feel it too. Please Please look deep into your heart and ask God to help you. If you ask Him with honesty and sincerity He will not only make it clear what you should do but He will give you strength to do it.
My heart goes out to you, Palesa, as I was in your shoes at the age of 17. I felt pressured to have an abortion, and I was so, so, so scared of raising a child on my own. I knew in my mind that it was my baby inside me, but another part of me (the scared part) kept telling my head that this was a problem that needed to go away. I never once even considered having the child and giving it up to be adopted by a family who could give the baby a wonderful life, lots of love, and would have the financial resources to take care of his/her needs. I made the decision to have an abortion. I am 58 years old now, and I can, without a doubt, tell you that that once decision sent me into a downward spiral for the past 40 years….my entire adult life. I started drinking, using drugs, partying, having sex with whomever and whenever I wanted to, and I just kept getting more and more depressed. I never even realized that all this behavior was due to the abortion and how it so deeply affected my soul. In fact, I never made the connection until just a few years ago. Thanks to Jesus, I am forgiven for that sin! But it has taken me many more years to forgive myself and stop thinking of myself as a worthless human being. I guess I’m telling you all this because I want you to think very hard about the decision to abort your own child. Yes….the problem will go away….physically. However, there are always consequences for every decision we make in our lives. Try to think beyond how this is affecting you today, and, instead, think about how the consequences of whatever decision you make today will affect you for the remainder of your life. I am praying for you, sweet girl!
Palesa, I have been in your shoes…and chose abortion. Worst mistake ever. Years of bondage..there is help out there for you.. Praying that God will protect you and your baby.
Been in your shoes.
Dear Palesa,
My wife and I are praying for you. God is bigger than all this. Stay strong. We are with you.
Love,
Mark and Kate
Palesa, I am praying for you. You are brave for reaching out for help. May God richly bless you and your baby.
Palesa, I am praying for you and so are many other people! There are many people and groups who can help you, your child, and your family. Have you checked OptionLine? https://optionline.org/
How brave and strong of you to reach out to someone during this time! You should try to google a pregnancy resource center near you — they’ll offer some good resources and help on all your options. Wishing you the very best, brave Palesa!
Your child will be your consolation. You will fall in love and your life will be blessed!!!! Seek help through a pregnancy counseling center. if you really don’t feel as though you can nurture this child then there are so many people who want to adopt babies. Give your child a chance at a better life. Just don’t kill the baby. The child does not deserve this.
Hi, I’m still a learner and 17 Years old I’m pregnant and i don’t know what to do my boyfriend has a 5 month old baby already and my mom doesn’t like him and i feel having an abortions is the only answer but I’m afraid of it’s effects. Please i really need help because I’m really scared and underage but worst of all I’m not sure if I’m ready to be a mother yet.
Dear Palesa,
I understand how overwhelmed you feel. You are right to be concerned about both the physical and emotional effects of abortion. Please read about the risk factors that identify women at greatest risk, as it is likely that you fit into one or more of these higher risk categories. That’s also a good page for your mother and boyfriend to read if they think abortion is a good idea.
Palesa, don’t do it. It’s not worth it. And in the long run, you’ll be much happier with the child you love than you will ever be trying to cope with the fact that you had an abortion.
Regarding your fear about not being ready to be a mother yet. Here’s a secret. No one is ever ready. We learn to be good parents only through on-the-job training. You’ll do fine. I’m not saying it will be easy. It will take work and sacrifice, but you will grow and value it all and become a better person because of every sleepless night and sacrifice.
Read some of the testimonies of women who have been were you are and wish they had been wise enough to turn away from abortion.
You can do this! Don’t give up hope. This will change your life, of course. But in good ways. An abortion will change your life, too, but it will drag on you and bring you sorrow. It looks like the easy way out. But it’s not. Once you became pregnant, your life was already permanently changed. Ready or not, you are a mother now. The only question is whether you will be the mother who can treasure your’s child’s laughter or a mother who will cry because you never had the chance to hear that laugh, or hold that little hand.
Be not afraid. God will bless you through this child. There may be a time of testing, and a time when you need to be strong and hold onto the hope and faith that everything will turn out. But you can do it!
You’re in my prayers. Please keep in touch and let us know how you are doing.
There are people who will help you Palesa. And I’m praying for you. Give this whole thing to God and ask him to direct you. He will be faithful and will always help you do what is good and right.
Dear Palesa:
I’m Lisa and I just learned about your difficult situation. I know that you feel terrified, alone, helpless, and overwhelmed at this time. You are right to be taking this seriously. You are faced with an awesome responsibility, no matter what you choose.Please know that no matter how you feel now that are are not alone. You can reach out for help and I hope and pray that you will do just that. Your boyfriend can also get help. I am listing resources below. Please consider a few!
If you need a place to stay, text SHELTER to 313131.
If you are being abused, call 1-800-799-SAFE (7233).
You can text PREGNANT to 313131.
You can text “Helpline” to 313131.
You can call 1-800-712-HELP (4357). Counselors help match you with a pregnancy help center in your area. THey can help your boyfriend also.
If you are despondent you can call: 1-800-273-8255.
If you don’t want your parents (or anyone) to know about your baby, you can surrender this helpline without fear of prosecution. Call: 1-866-99BABY1 (1-866-992-2291).
You can contact Birthright. They exist to help girls: 1-800-550-4900.
You can visit: http://optionline.org
You can visit: http://www.standupgirl.com
You can visit: https://www.care-net.org/find-a-pregnancy-center
Prayers 4 You N 4 all Involved!
Lisa
I WAS RAPED AND MY MOTHER DID NOT WANT ME TOO HAVE THE BABY. NO ONE TOLD BUT I KNEW IT WAS WRONG. SHE IS GOOD NOW. IF YOU NEED TO TALK SEND ME AN EMAIL
Please hang on, Palesa, you feel deep down not to do this, you love your baby and your family will too.
We are all praying for you and for the life of your child. I pray for strength for you to do this.
My girlfriend had an abortion 5 days back but she is weak and lost her apeptite so plz help me to overcome this.
Hello, I’m so glad you found our site. I’ll try to give you some help, but please note that I can’t give you medical advice. If your girlfriend is having physical problems (especially anything beyond what the clinic told you to expect, or if she is having symptoms this long after the abortion) then she should see a doctor to make sure she is okay. If there is anything that seems to be very serious or life-threatening, get her to a doctor or emergency room right away. I really can’t tell you what symptoms are normal or not, so you should seek help for her or persuade her to seek it if you are feeling concerned.
Emotionally, she has just been through a huge ordeal and may not be able to process the situation yet. She likely needs support and care from you, and you need to remember that you too might be feeling the fallout from this and need support as well. Obviously, I don’t know the circumstances that led to the abortion, or how either of you are feeling about it. Even if you felt okay with the decision at the time, sometimes troubling emotions and regret don’t hit until afterward. You can talk to your girlfriend about it when she seems ready, but I wouldn’t force the situation if she doesn’t want to discuss it.
What I would suggest also suggest is that you contact a group that offers support for those who have been through an abortion (note that these groups are for women and men, so they can help you too if you need that). These groups offer free, confidential and non-judgemental counseling and support, or just a listening ear if you need it. In any case, they may be able to help you address your concerns about your girlfriend and figure out how best to help her.
You can find a list of such organizations on our healing page. If you don’t feel ready to talk with someone over the phone, you can contact Rachel’s Vineyard by email or get help through text (text “HELPLINE” to 313131) or chat from OptionLine. Rachel’s Vineyard also has a Q&A section where you can post and read questions about healing.
Palesa, I have a lovely 11 year old adopted granddaughter. Her 17 yr. old birth mother came from almost the exact circumstances as you. We are so grateful that she was so brave to give life to her child. It was a private adoption. She chose our daughter and husband from three applicants. It was an emotional moment when she laid the baby in the arms of her new parents, but she knows she will see and get to know her daughter again one day. She will never have to live with the pain and regrets of ending the life of her own child, and she knows that that little girl has the love and guidance of two mature parents. I pray that you will make the same decision of bringing your baby into the world as a blessing to a specal couple who are able to be the parents that you are not able to be at this time….and that one day you will be able to marry and be the mother God created you to be. Our granddaughter knows she’s adopted and looks forward to the day when she will be able to meet “the mom who God chose” to bring her into the world to be loved and raised in our family.
I pray that you also will give yourself the gift of assurance that one day, you and you child will meet again. There’s nothing more wonderful to look forward to on this earth.
You are in my prayers. Don’t be afraid, God has His arms around you.
Hi,thanks for the good information to people about abortion.my question is, my first cuz had an abortion last week ,only me I leant about it though she don’t khow I khow .my concerned is she is only 20yrs, am fearing for her future life and chances of her doing it again since they still together with the boyfriend.
Should I alert one of family doctor to try to discuss and find out if there is any kind of help she need to given
I wouldn’t recommend sharing her secret with others. But I would look for opportunities to let her know that if she ever needs to talk about it or is struggling with it, you’re there to listen and try to help. And if she does ever reach out, encourage her to seek help from a [https://afterabortion.org/help-healing/ post-abortion healing program]. Don’t push her. Don’t make her feel like you are judging her or expecting her to feel guilt. Just be there for her if and when she does want a sympathetic ear.
In have had abortion five years ago and I don’t know whether some of the foetus left inside. Ever since I did the abortion have being reducing weight. What should I do. And my period is not flowing properly
Please go see a doctor. You are in my prayers.
Thank you and God bless you for the healings and helps you are bringing to the victims of abortion risks. I now want to address my fellow youths, please avoid abortion and every thing that will lead you into it. Though your doctor may tell you that there will be no problem committing abortion, but the truth is that it is not safe at all. If there be no complications now, it will still come later. Not to talk of the guilts of blood shed if you have conscience at all. Please avoid pre marital sex and be safe from all the possible abortion risks. God bless you.
What measures could take when I found that I can’t get a baby due to abortion?
Has a doctor told you that complications from a previous abortion prevent you from being able to become pregnant again?
Hello sir,
Already I had 2 abortions in the same year.now I am pregnant after did my second abortion two months back. I am having financial and also carrier vise settling process. So now I want to do abort.is it safe to me to do.is there any health issues in it… I need your advise.
Risks increase with each abortion. Multiple abortions are linked to higher rates of death, reproductive problems, depression, anxiety, addictions, post-partum depression, and more problems parenting children. Also, you may be trapped in a cycle of repeat abortions. The only way out is to carry a pregnancy to term. I would strongly advise against another abortion. Please look for help with any expenses for carrying the baby to term, whether you decide to keep her or place her for adoption, from a pregnancy help center or church. Where do you live? Perhaps we can help find you some local support.
Am pregnant I don’t know what to do cause my boyfriend dad is very strict the goes to my dad we don’t know what to do we are considering abortion
First thing: please read about the risk factors that studies have shown can identify which women will have the most emotional problems after an abortion.
If any of these risk factors apply to you, I strongly discourage you from having an abortion just to please your parents. Trust me. Parents aren’t happy with surprise pregnancies. But they get over it. Especially when they see that beautiful child. They will adjust. Probably, faster than you think. A lot of the “gruff” of parents is to convey their hope that you won’t have children “until you’re ready.” But once you’re pregnant . . . well, they can’t argue with the fact that having a child is the only thing that ever truly makes us “ready” because now we really do have to be responsible for another person.
You can do this! I’m sure you will be a great mother . . . precisely because, as all mothers have learned, there is lots of on the job training.
Don’t let yourself feel pressured into an abortion to please others. It’s the surest sign of regrets and remorse that can last a life time.
Hi I need help I am 8 weeks pregnant I am to have an abortion tomorrow morning this will be my 6th abortion in period of 9 years my last was a couple of years ago. I’m not proud of myself I’m act very ashamed of who I am and what I’ve done. I have 3 kids already and I barely make it with them it’s just over whelming the thought of bringing another baby into the world I should have been more careful. I’m scared I’m scared of dying I’m scared of what impact this is having on my body emotionally I’m numb to everything. But physically my health is poor. I just don’t know what to do
Dear Nikki,
Please reach out to one of the post-abortion healing programs listed on our help page. Or more than one. Keep calling and interviewing until you find the right one for you.
Repeat abortions are especially harmful, both physically and emotionally. They may also indicate a pattern of self-punishing behavior that you need to sort through in counseling.
I would, of course, also encourage you to cancel your appointment today and meet with women at the local pro-life pregnancy help center. Maybe they can give you the immediate help and resources you need to break the cycle this time. I know it is hard to imagine handling a fourth child, but give them a chance to help you find a way.
You are in my prayers.
I had an abortion last year for my boyfriend because I was scared by then he still had issues with the mother of his child….now everything is sorted out and I hav introduced him to my family and last week we just both found out that am pregnant now am scared of mum and dad and my bro who is paying my tuition fees and we have considered another abortion with him coz hz nt working at the moment and we re worried my bro myt stop paying for my school tho we re both having second thots about it….pliz help
Hello Deedy,
I’m sure you are very scared right now. But please don’t feel like you need to rush into anything! First, having a baby doesn’t have to be the end of the world — it can truly be a joy! Yes, even in circumstances where you are not prepared and don’t know how to handle it, or how your family will react.
The first thing you should do is reach out to someone who can help. I don’t know your family situation and it sounds like you are scared about letting them know. However, there are many organizations out there that support women and couples during and after pregnancy. They can help you and your boyfriend sort out your plans. This page has a list of organizations nationwide who offer options counseling, practical support, relationship help and more to women who are pregnant. If you are outside the U.S., contact us at elliotinstitute@gmail.com and I will try to find a local organization that can help you.
Also, you shouldn’t have to quit school because of a baby! It can be a hard path but women can and do succeed at this. If you are in college or university the Pregnant on Campus Initiative and Feminists for Life’s College Outreach Program may be able to help with resources, information and support to help you complete your education. FFL also has a web site called Raising Kids on a Shoestring that has a ton of information on free and frugal resources, solutions and practical support for pregnant women, expectant fathers and parents.
I’m guessing that since you are having second thoughts that your first experience with abortion wasn’t all that great. Not only do you not have to go down that road again, but if either you or your boyfriend is struggling there is hope and healing available. Many of the pregnancy help organizations listed on our help page also offer post-abortion support and counseling for women, men and couples. They can help you and your boyfriend heal from this experience and work out any issues this may have caused in your relationship. There are also organizations dedicated to helping after abortion such as Rachel’s Vineyard, which also offers support through email.
You and your boyfriend need to listen to your hearts, find people who can support and get real information about your options — and you do have options even though it might feel like you don’t. Don’t let yourself be pushed into making a hasty decision you might regret.
Hi, am Xtine.. Am 5wks pregnant and my guy has denied being responsible for it, he has suggested I do abortion and if I will keep it it’s upon me,, not to bother him.. Since last week he hasn’t called me and if I try reaching him my call can’t go through?? I need your advice pls
Hello Christine,
Don’t feel like you have to have an abortion just because your boyfriend wants to get one. You have rights and options. It is actually illegal for him to try to force you to abort or not to support his child. You need to talk with someone who can help you find out all your options and make the decision that is best for you and your baby.
This article “What to do if your boyfriend wants you to get an abortion,” has a lot of great advice and suggestions as to how to handle this situation. You should also contact a pregnancy help center as well. This page has a list of organizations nationwide who offer options counseling, practical support, relationship help and more to women who are pregnant. If you are outside the U.S., contact us at elliotinstitute@gmail.com and I will try to find a local organization that can help you.
Please know that you are strong enough to get through this. Don’t feel like you have to give in or that you can only take the path your boyfriend wants you to take. Things may seem frightening right now, but you are not alone. There are people who want to help and support you and who care about you and your baby.
Having an abortion to satisfy the demands of a boyfriend just puts you at higher risk of greater emotional problems later. If he refuses to be part of your child’s life, that will be his loss. The law will require him to pay child support, but it can’t require him to be a good dad. And if that is the way he is, you are better off without him. You can and will find a loving husband who will be a good father for your children. Meanwhile, just concentrate on being the best mother you can for your child…including protecting your child from his father’s short-sightedness. Perhaps, as the pregnancy progress or after the child is born, it will soften his heart and he will love his child as he should. But for right now, he is lost in his own selfishness. Don’t let his current blindness push you into something you know is wrong. You will never regret having your child, nor will all the other people who will come to love your child…grandparents, friends, future spouse . . . and eventually, the child’s father. You are making the right choice.
i think that people should not get abortions because they re killing their babies and that is a bad thing.
Hi Mykia,
Thanks for your comment. It is always a good idea to have information available to help those who need it. Many women are pressured or coerced to abort, or don’t know about other options available. Our pregnancy help page includes a list of organizations that provide help to women and their loved ones who are pregnant and need support.
There are also organizations that provide support and counseling to women, men and families after abortion. You can learn more about this on our post-abortion healing page.
It’s a good idea to hang on to this information to pass on to anyone you know who might need it.
hello. i’ve a friend who has undergone one abortion before for almost four years. she was really terrified and until now, she’s still afraid..mostly, she’s afraid if she can’t bear any child anymore. because her husband and her were planning to have a child, they’ve tried it for several times,but still she’s not conceiving. She told me that she haven’t gone to any doctor since the abortion and she’s afraid that complications were present in her uterus. and she can observe a foul-smelling discharges inside her.I REALLY NEEDED your help urgently for me to advise my close friend.please
Dear Kyry,
Your friend should see a doctor if she is having any kind of problems. If she is having complications and they are not treated, it could create more problems later on. She should also definitely let the doctor know about her abortion history so that the doctor can address any issues this might have caused. I would really encourage her to do this even if she is afraid, so that any problems she may be having can be treated. It could also be that there is nothing wrong or it is simply just taking her a while to conceive, but seeing a doctor could help put her fears to rest.
If you would like to find out more information for her or find a pro-life doctor (in the US) that can help, you might consider contacting the American Association of Pro-Life Ob/Gyns. They won’t be able to diagnose any problems from a distance, but they might be able to give you and your friend some information to put her at ease.
Also, if your friend is struggling after abortion (either with fears about not being able to have a child, feelings of grief or shame, etc.) she should know that she is not alone. There are ministries out there that can help. They offer free and confidential support and counseling to help her work through any fears or negative emotions she might be having after abortion. These counselors are kind and non-judgemental — sometimes they are other women who have had abortions so they know exactly what it is like. You can find out more about this on our healing page. If you live outside the U.S., you can contact Rachel’s Vineyard for more information by email. They have healing organizations in a number of countries and also offer support through email.
I hope this helps! It sounds like you are a very good friend who really cares and wants to help your friend, so I would strongly encourage you to share this information with her and reach out to people who can help her.
I feel in love with a wrong person and became pregnant 3 years ago. He wasn’t supportive, and also due to my families situation, I had to undergo abortion without any option, I am unable to reveal this to anyone around, as it would create a huge issue in my family. Now am 23 my parents had found the right guy for me and am happily got married 1 year before. Now we are plan to have a baby. So before that we went hospital to know my health condition. And gynecologist prefer to anxioum to conceive scan.My worry is that, will my abortion affect my future? Can doctor identify that i have undergone abortion in my past ? Am completely worried about it. Can someone help me on this ? Also, my husband don’t know about my past. Kindly help me with my question.
Dear Abhija,
First of all, please know how that I’m very sorry you believed you had no other option and that you had to have an abortion. I’m sure this is a sad and difficult situation for you. If you are struggling, please don’t try to keep this all to yourself. Is there someone you can trust to talk with about it, such as a minister or pastor, without telling your family? I don’t know where you live, but there may be a pregnancy center, pro-life organization, or other ministry in your area that offers support to women who have been hurt by abortion. You can also email Rachel’s Vineyard for support by email. I would really encourage you to contact them as they give you counseling and support.
As for your question, your doctor probably can’t tell if you have had an abortion unless you tell him. That being said, it is usually a good idea to tell your doctor as it might help him or her to know about any issues that can affect your health or fertility. In the U.S. at least doctors are not supposed to share that information with anyone.
I don’t know you or your husband, so I don’t want to give you advice as to what you should tell him. Keeping something as important as this a secret because of feelings of shame or fear is usually not good for a marriage. However, only you know how this could affect your relationship with him. This is why I would really encourage you to contact Rachel’s Vineyard or another trusted counselor. You can tell them about your situation and they can help guide you about what you should do. Please know that you are not alone, that there are people who care and want to help.
You can find out more about post-abortion counseling here, including a list of organizations in the US. If you live outside the US, you can email me at elliotinstitute@gmail.com and I will try to help you find an organization in your area that can help.
hi
my friend had an abortion some 3months ago and she got pregnant again. she wants to have another termination. she is 19years what can i tell her
Hi Debrah,
Thank you for trying to help you friend. Do you know the reasons why she is seeking another abortion? Knowing that and helping her address those issues can help. It sometimes happens that a woman might get pregnant soon after her abortion because she wants another baby to “make up” for the one she lost, but she ends up aborting again because the problems that led her to have the abortion in the first place are still there.
Your friend needs you to be there for her, to talk to her, listen to her and know that you want to help. Encourage her to discuss why she wants or feels like she needs to have an abortion and see if you can work together to find solutions so she doesn’t feel like this is her only option. Remember that right now she is probably not in the best position to making big decisions, as she is likely feeling scared and overwhelmed.
Encourage her to take time to explore all her options and find resources and support to help. You can contact OptionLine or visit this page for a list of organizations that help women who are pregnant — all the help they give is free and confidential. If you can, offer to go with her or help her contact them so she doesn’t have to do it alone.
Also, if you friend is being pressured to have an abortion she doesn’t want, this article has lots of helpful information for women in that situation. She can also contact the Center Against Forced Abortions for legal help to stop others from pushing her to have an abortion.
I am newly married after 10 days my wife get pregnant both wanted abortion because we are not ready yet what should I do please suggest there any risk in abortion please tell me
Hello, Absnns, thank you for coming to this site! It’s normal to not feel like you are ready to have a baby and to be worried about what this means for your future. It’s okay to feel that way. But what you shouldn’t do is let those worries and any difficulties you are having right now drive you to make a decision you might regret. Abortion is a decision you can’t undo, and it’s hard to make good decisions when you are facing a crisis.
Abortion does carry risks to your wife’s physical and mental health, as you can see from this page. There are also risks to your relationship as well. Many couples have problems in their marriages or break up after abortion. It can cause resentment, difficulty communicating, grief, regret, pain and other problems that can make your relationship fall apart. You may not feel ready to have this baby, but do you really want to risk putting your wife through something that could hurt her (and you) and lead to problems in your relationship?
I would suggest visiting this page to learn about the problems people might have in their relationships after abortion, and also reading through the comments (especially the comments posted to Samantha) to hear from others about their stories of how their abortions affected them — and also to read about how their lives turned out when they had the baby. You might find some good information and encouragement here. Also, the Silent No More Awareness Campaign also has lots of stories from those who had abortions that talk about the impact abortion had on them on their relationships.
Above all, please seek out support from an organization that can help you. I don’t know where you are located, but there may be a crisis pregnancy center or other organization in your area that offers free and confidential support for women and their families during and after pregnancy. They can help you get information about your options, resolve issue that make you feel like you aren’t ready to have the baby, and find resources that are available to help you. Visit the pregnancy help page for more information and a list of organization that offer this kind of support. If you are outside the U.S., you can email me at elliotinsitute@gmail.com and I will try to put you in touch with someone that can help you.
What about seeking help and support from your families, friends or a church? You may find that there are more people than you think that will be happy about your pregnancy and willing to help you.
Please don’t rush into making this decision. You need time, information, and the right support. Your wife needs you to be there for her and your child. Please seek out help and support from people who care.
Hi,
My friend had 3 abortions.2 abortions in a year and the 3rd one after a year. she was forced to do it but she didn’t want to. All the 3 babies she had was not more than 1 month old.
I have just read the article in yr website n it said that the risk of death is very high,does it include death in pregnancy or natural?she is afraid of it. she is planning to get married in few months? Can she ever get pregnant again? What are the steps she needs to take concerning this?
Hello Maria, please encourage your friend to speak with her doctor and tell him or her about the abortion if she has concerns about her health or fertility. They will be best equipped to advise her and treat any health issues she may have. If you are in the U.S., a good resource would be to contact the American Association of Pro-Life Ob/Gyns to find a doctor who can help her.
Yes, research has found increased rates of health problems for women who have had abortions but it doesn’t mean your friend has them. Our intent is not to make people afraid but to provide information on what the research is finding. Your friend needs to talk to someone who can help her put her fears to rest.
Also, if the abortion was unwanted, she might be struggling emotionally as well. She is not alone and there are groups that can offer emotional support and a safe place to talk. You should encourage who to contact someone who can listen and provide counseling and support to help her heal. You can find more information on this on our post-abortion healing page (or email us at elliotinstitute@gmail.com if you are outside the U.S.).
hello
I’m 26 years lady. I already did 3 abortions and again I have pregnancy. I used some vaccinations against rubella and doctor told me till three months you should have pregnancy, it only have 2 month of vaccinations. I’m so worry about that what I do? hoping your good suggestion. exactly I do not want to abort it but scared about hamperness of vaccines.
There is very little risk that the vaccine will cause any harm to your baby. Doctors recommend to avoid pregnancy for even a small risk. According to one authority, the risk is all theoretical; there is no evidence that the vaccine has ever caused rubella related complications in babies . . . even when women are vaccinated during the first few weeks of pregnancy!
The doctor’s advice was just that . . . a recommendation on the level of “why take any chance when you can just avoid pregnancy.” Now that you are pregnant, stop worrying. Trust God. Trust your own body.
On a side note, I’d also encourage you to find help with any emotional hurts you may have over your past abortions. Talking to a supportive counselor, pastor, or friend may help you overcome issues that may make it harder to be the best mom to your children that you can be.
You are in our prayers. Please don’t hesitate to write again if you need more advice or encouragement. We’d also love to hear about your progress! Be not afraid!
My girlfriend did abortion because i have three kids, she is unemployed and i dont have a house last year.
Today we have moved away from it, we never discuss is and that was our agreement then.
She did murder for her convinience and i am totally broken even though she is not the first girl who aborted my child, the problem with her doing it is – “i love her” but ever since she did it i’m no longer sure whether we love each other or we are just sex partners who play dangerous sex games by not condomizing.
Hi Koki, it sounds like you and your girlfriend need help to work through this. What a painful and devastating loss — I am so sorry for what you have been through. Not discussing it or seeking healing will only do further damage to your relationship — you need to talk, to get things out in the open and make good decisions about your relationship and your future. But you shouldn’t do it alone. There are organizations and support groups out there who can help. If you girlfriend isn’t willing to go with you, you should seek help for yourself — otherwise the resentment and pain you feel will just continue to grow. Please visit our healing page for more information on finding free and confidential, non-judgmental help after abortion. You can also find articles and information for men here. You are not alone — there are people out there who know what you are going through and want to support you.
Great information that every woman should know about. Killing an innocent baby who has not yet opened eyes in this world does not deserve death……. Stop killing babies..
Why killing the innocent soul due to your fault. Avoid abortion, love your baby.
A guy approached me today narrating how he got a lady pregnant, although am working in a hospital as scientist. But I actually booked an appointment to talk it over with them. The duo have a strong determination to abort the barely two weeks old foetus. What strong advice should render to make the give up their plan? Thanks
I would encourage them to carefully study the risk factors which identify the women who are most likely to suffer more severe psychological reactions to abortion. It is likely that the woman has multiple risk factors.
They should also look at the studies that demonstrate the elevated incidence of psychological and physical problems associated with abortion, including reduced life expectancy.
Bottom line: Abortion can make sense to the head, but it is not easily reconciled at the level of the heart. Many women will end up regretting their abortions; very few ever regret giving birth to their children, even when the child was unplanned.
All the reasons for abortion make sense here and now, at this moment, but the reasons won’t stand up against the self questioning and self rebukes which follow. Abortion doesn’t turn back the clock. It doesn’t make everything the way it was as if you never became pregnant. Their lives are already changed. They are already parents of a real, living human child. The question is whether they will ever hold the child, or whether they will always wonder about what it would have been like to hold it.
The idea that abortion will turn back time is one of it’s most dangerous lies. The choice is not whether or not to be parents, but whether or not they will be parents of a live child or an aborted one. While a live child involves burdens, and aborted child is not without it’s own costs.
After reading it, abortion is never the answer, there other ways through it. don’t do it, it’s not if it is safe or not, it is that you are killing someone who is innocent, look, if every child had a decision between to be “born” or “aborted”, I guarantee 100% of the babies, the would say to be born.
To those whose parents have threatened to throw you out if you don’t
murder your baby: what would your reaction be if they said you couldn’t
stay unless you shot your boyfriend? It’s he same thing, you know. Only,
abortion is easier because you don’t have to look your victim in the eye,and you can hire a hit-man in a white coat cheaper than his mob
counterpart.
Your parents are telling you to do an evil thing, whether they think they are or not. And they are taking advantage of the fact that you are
scared and feel alone and helpless. That may not be their intent, but that’s what they’re doing.
You are not alone There are people out there who will help you through
your pregnancy and even give you a place to stay, who will arrange
adoption or help you adjust to being a single mom.
Go talk to your local crisis pregnancy ministry, state or city right-to-life organization, or just drop in at your local Catholic church (they’re the ones who have the most aggressive pro-life ministries)
and tell them you need help.
Or, for that matter, you can write me, and I’ll refer you to people
who can help.
You are not alone. You are not helpless. You have friends, you just
haven’t met them, yet.
You can reach me at: arimathea@priest.com
Blessings,
Fr. James Rosselli
St. Joseph of Arimathea Orthodox Church
and House of Prayer
La Porte, Indiana
Change the abortion thinking
I have 5 months old baby . Unexpectedly my wife have pregnant in this month. What should we do ?
Is abortion will better options.
I strongly discourage an abortion. It will expose your wife to much greater mental health risks and long term physical risks, including a shortened lifespan. It is also likely that she has multiple risk factors for more severe reactions than other women. Finally, having an abortion may make it more difficult for her to bond with and raise your five-month-old baby.
Please trust that this unborn child is a great gift to you, your wife, and your already born baby. It may be hard work caring for two little ones, but they will be the best of friends and will bring joy into your life that you will never regret. An abortion, on the other hand, will leave all of you with a life time of regrets.
Hello, my girlfriend had an abortion last year november, but since then her period has not been a regular cycle like it used to be,,, what should she do?
thanks for the information
my girlfriend want to go for abortion because her mother says she cant stay with her if she doesnt do abortion and i feel so helpless because i dont have a job and my girl friend she is 19 years old and am 20 years old. i dont know wht to do please help me, from South Africa ….
Hi Dan, I don’t know where you are located in South Africa, but there are organizations that can offer help to you and your girlfriend to have the child. She doesn’t have to abort, even if she feels like she has no other choice or if her mother is threatening to make her leave. I have included a list below of organizations that offer free and confidential help. Please contact us again if you need more help!
http://ramahinternational.org/help-in-your-area/international/
http://www.optionsgeorge.com/
http://www.lifechoicesbenoni.co.za/contact_us.html
http://birthright.org/en/landingpage/lp-johannesburg
http://www.joytothenations.co.za/heart.php
http://www.crisispregnancy.org.za/
http://www.pccofhope.org.za/contact-us.html
http://healthymomandbabyclinic.com/crisis-pregnancy-counselling.html
http://www.choices.org.za/counseling.html
Ennitan,i had an abortion four times,when I was in school because then I am not ready for a baby but now that am married, a years ago have been praying to God to forgive all my sins bcos then I don’t know what am doin,I just want to be sure if I can still concieve.
I had an Abortion before 4 month when i was 6 weeks pregnant. For last one month i am trying to conceive but i can’t though i have regular period every month. Can you please tell me the reason behind that or any suggestion. I am really worried.
Hi Ella, if you have any concerns about your health and your ability to conceive you should visit a doctor. Be sure to let him or her know about your medical history and any symptoms you are having. The doctor should be able to tell you if you need to be concerned and what treatment might be available if you are having problems.
I had a an abortion eariler this year when I was still a student studying my master degree. My boyfriend was supportive and tried to persuade me to keep it, but I felt that I didn’t have the capability to bring up a baby. Also because I am from a very conservative culture, being pregnant before marriage is considered to be a huge shame.
Due to all kinds of pressure, I aborted that baby. Now half of a year past, I become more and more anxious and frightened psychologically. I feel that it was a huge mistake in my life and I feel shameful for myself. I can’t talk to anyone about my true feelings I feel very helpless sometimes. Sometimes in my mind I always blame my boyfriend for this, I doubt that it is him make me pregnant on purpose. He knows I am not planning to be pregnant but he sometimes insist not using condoms. His selfishness and this abortion experience make me lose confidence in this relationship too. I really wish nothing happened ever. 🙁
Please read on page with tips on finding post-abortion healing support. It sounds like you may not be in the United States, so programs may be harder to find. But some Christian churches and pregnancy help centers (if any) in your area may be able to refer you to a program or support group.
You are in our prayers.
Ive done an abortion 1 week ago. my bf didn’t ask me if its ok with me to go abortion. we got aborted the baby,i didn’t contradict his decision..after 3 days I got confined to the hospital to do an operation because there were retained products of conception and blood clots in my ultrasound. and now 4 days after I got confined in the hospital ive been having dizziness and eating disorders and afraid of getting pregnant..what should I do?
I’m not a doctor. Regarding any physical symptoms, you should go see a doctor your trust if you are experiencing anything that concerns you.
Regarding your emotional recovery, at some point you may benefit from seeking the support of other women who have been through an abortion and found healing by contacting a post-abortion healing program. Please don’t settle for just “getting by,” much less “suffering in silence.” Get help to work through your feelings of loss before they sink in deep and begin to fester.
hello,
am 19yrs old, my girlfriend is pregnant and she wants to abort the child as we are not mentally and financially prepared. should i support her in this decision??? she is 21 yrs old.
Hi Adush, thanks for posting. I don’t know your exact situation, but you and your girlfriend are probably pretty scared about the future right now and about what having a baby could mean. Maybe other people are scared for you too and telling you that you can’t have a baby or abortion is the only thing to do. You sound like you want to be there for your girlfriend, so let her know you care about her and your baby. This is a huge, life-altering decision and you should find out everything you can, talk with people who will tell you about the risks and other options you might have, and offer you good support and resources.
Here are some places to start:
Find out about the risks of abortion before you have one. Abortion clinics and even your girlfriend’s doctor might not know or give you this information. They might tell you that abortion is safe and there is no risk. But aside from the physical risks, it is widely accepted that certain women are more likely to have problems after abortion. You should check out this page and see if you and your girlfriend fall into any of these categories: If you do, it might mean that you could have a harder time dealing with the abortion afterward. https://afterabortion.org/2011/risk-factors-for-psychological-problems-after-abortion/
Find out about other options. There are many resources out there to help that you might not be aware of. I’m not saying it will be easy, but many women and men who go through abortions end up with regrets afterward, even if they think or were told it was the right decision at the time. Please visit here for information on pregnancy support centers: http://www.optionline.org/get-help.
There is also an organization called The Nurturing Network that can help with things like housing, finding a job, staying in or going to school, etc. http://nurturingnetwork.org/ All the help they give is free and confidential.
I hope this helps. Please know that, no matter what anyone says, you DON’T have to have an abortion and there are other options — and people who will help.
I am having cramps, serious cramps but no sign of period and pregnancy…. help?
I’m not a doctor, nor could a doctor diagnose you from just a report of cramps. I strongly urge you to see a doctor or seek nursing help or a referral through a pregnancy help center.
I had an abortion 2yrs ago bcoz the baby died inside my womb and it’s been a week dead. A midwife provided a Meds to abort the baby. The baby came out just like a normal delivery except that baby is just 6months old and dead. Now, I have health issues. Been having Eating disorders and lately being sickly. Also, been trying to get pregnant again but no luck. What should I do? I’m honestly very worried. Is it still possible for me to bear a child?
I’m not a doctor, but from everything I understand there is no reason to believe that you can not bear a child in the future. It is possible that your eating disorders are making it harder for you to become pregnant again.
Hang onto hope. Things can get better and you may soon have the baby you desire. If you have access to a doctor, go see him or her and discuss your situation. For some people, it may take a year or two of trying to become pregnant. You might want to start tracking your cycle to see when the most fertile days are to increase the chances of becoming pregnant. There are easy ways to become more aware of your fertility that you can read about here. and elsewhere.
I am 34 yr old I have sufgering from pcod i had 3 abortions in 5th month I have one child 6yr old for the first baby I did cervicalcerclage but after other pregnency I don’t .for the second pregnencyeverything is normal up to 5th month but after doctor told me that it is dead inside. After that pregnancy immediate two month s later I had another pregnancy it is also normal up to 4yh month but it is also dead in the last of fourth month again they did the abortion. I notice the problem when I g
ot pregnency I suffer from light chill and fever please tell me having all these problems shall I take another chance of pregnancy
I’m very sorry for your losses and the health problems you have been through. I would suggest talking to your doctor or getting a doctor’s opinion on any specific health problems you have. You might also want to check out the American Association of Pro-life Ob/Gyn web site at http://www.aaplog.org.
Thank you for this information, I will be using some of these facts to convince people to be against abortion.
I have done 2 different abortions which am forced to do 2 years back and now am having psychological trauma and always have this guilty feelings if I have not develop any complications especially in my future pregnancy, and will always need an advice on how to find out if there is any and means of solving pls
Please read our page of tips and resources for finding a post-abortion healing program.
Regarding your future pregnancies, when you become pregnant be sure to tell your doctor that you have a history of two abortions and that you are concerned about the heightened risk of premature birth and miscarriage. There are techniques that can be used to reduce the risk of miscarriage or premature birth and a doctor who is aware of your increased risk can take these appropriate steps.
Don’t give into despair. Find a post-abortion healing program where you can get the emotional support and help you need to regain a sense of peace in your heart. You will never forget the children you’ve lost, but you can work through the grief and find a sense of peace.
Yes, there is!
You need to get right with God. People often view God as some cosmic
Bad Guy, Who is out to zap them for doing wrong. Nothing could be farther
from the truth.
God loves you. He desires your healing and salvation. In Christ, you will find both.
For your specific situation, I’d suggest you get in touch with your local Women’s Care Center or any church affiliated with your local Right-to-Life office.
I am so happy that you have said that, God bless you man. I support you very much
Probably that´s right. I´m atheist, but in some cases I encourage people to go to the church, or a buddhist center, a mosque, or something similar. I believe that religion is something that is more than salvation, is something related with direction, counseling, hope. Hope is what any human being wants to his/her life, and religion gives hope, so maybe it should be good in those cases.
MY BOYFREND FORCE ME TWO COMET ABORTION
Our prayers go out to you Florence. It doesn’t sound like your boyfriend is committed to loving you. It seems like a bad relationship. You deserve better. I also hope you will look into programs that can help you heal from the your past abortions.
Im strongly against abortions, BUT, i am a mother of a 2 yr old and 5wks pregnant with another baby. I think my boyfriend is trying to talk me into getting an abortion. I dont know what to do at the moment, because i can hardly take care of the child i have already from a previous relationship. I just need advice…
Please check out our pregnancy help page to find resources to help you with friendship, good advise, financial support, and more.
Don’t give into any pressure or manipulations to have an abortion. Ask him to read about abortion risks on our web site and to read the testimonies of both women and men. Help him to see that abortion is not a simple fix, as he hopes, but rather a negative choice that could damage both of you for life . . . especially because you are strongly against abortion. Asking you to betray your conscience, and your child, is not loving. He needs to stand up as a man and protect you and his child . . . not endanger both of you because of the misguided hope that abortion is a “quick fix.” Hopefully he will understand this once he educates himself.
In either event, whether he becomes supportive or continues to encourage the idea of having an abortion, you need to expand your support network by contacting a pregnancy help center and reaching out to friends and family members who will give you emotional support and who will reinforce your decision to protect your child and yourself from an unwanted abortion.
You are in our prayers. Please let us know if and when you boyfriend starts offering you the support you deserve. If he doesn’t, please let us know if you have found the help you need through a pregnancy help center.
am stressed up because my man want abortion
I’d suggest a few things.
First, call a pregnancy help line listed on this page to get support and advise.
Second, have him read some of the testimonies of women who have been hurt by abortion. If he truly loved you, he wouldn’t want to risk having you go through the same nightmare.
Third, stand strong for yourself and your baby. If he’s just using you, then it’s better to see through him now than after you have lost your child and your the person you want to be.
Don’t give up hope! Stand firm for what you believe.
You are in our prayers. Please call one of the help lines for support.
my man want me to abort
That’s because he doesn’t know how much it will hurt you emotionally, psychologically, and physically. Or (I hope it’s not true), he’s too selfish to care about what it does to you or the baby.
Stand up for yourself and the baby. If he’s a good man, his attitudes will change. He will get over the fears of having new responsibilities and will embrace the joys of being a good father. If he’s not a good man, you are better off without him. Don’t damage your soul, your heart, your mind or your body to satisfy the demands of a selfish man.
Keep your baby. In the end, your child (and future children) will be your greatest treasure and pride. Having an abortion will be your greatest tragedy that you will carry with you always. Choose the treasure, not the grief.
Ask your man to read about the risks of abortion. Have him read about the risk factors that put you at greatest risk. If he’s a good man and truly loves you, this will change his mind.
Please keep in touch. Let us know how we can help you.
You are in my prayers.
Do you want to hear from other women who have been in the same situation? If so, I will send out an invitation for them to add comments on the page where you commented and you should receive copies of their comments by email. (They won’t have access to your email address. But the website will forward their messages to you). Let me know if the advice of more people may be helpful.
Please pray along with me and also I will like to hear those testimony of others women thank you
This is a two-year-old post, but for those in similar situations, the
best route is adoption. It’s not a complex process, and you will have all the help you need along the way. Call any Women’s Care Center
office, or any Right-to-Life organization, for information. You will
be astounded at the amount of help that’s out there for you!
first of all if you can’t take care of the baby don’t abort their is adoptions My aunt is adopted and she is one of the best people in my family just last year i got to meet her birth mom and she was in a situation simler to yours but she knew abortion was not the awner instend she give the baby up to a family she knew would love and care for her. also thir is closed and open adoption so you could still be in your childs life